The molecular basis by which small amounts of HIV can initiate infection in the mucosa is not well understood. We have discovered that genital and rectal fibroblasts, amongst the most abundant cells of the mucosa, potently increase HIV infection of T cells. In contrast to fibroblasts, mucosal epithelial cells, which line the mucosa, inhibit HIV infection by apically secreting antiviral factors. Our findings suggest that abrasions in the genital and rectal epithelium may increase HIV transmission in part by allowing HIV to escape an antiviral environment to access the infection-favorable environment of the stromal fibroblasts. Ongoing research in the lab seeks to determine the molecular mechanisms by which stromal fibroblasts increase HIV infection of T cells, and conversely the mechanisms by which mucosal epithelial cells limit infection rates, using ex vivo tissue models. The effects of seminal plasma components, which we previously demonstrated markedly enhance HIV infection, along with sex steroids and microbicide candidates, are also being investigated in these model systems.
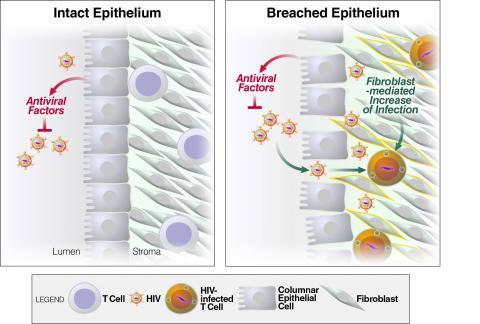
Model supported by our ex vivo studies on the effects of genital mucosa-derived cells on HIV infection (Neidleman et al, PLOS Pathogens, 2017). In mucosal tissues lined by single-layered columnar epithelia, such as the endometrium, when barrier function is intact, antiviral factors secreted by the epithelium can limit HIV infection. Breaches in the epithelium caused by physical trauma, ulcerative sexually transmitted diseases, or the effects of progesterone facilitate migration of HIV from the lumen into the stromal compartment. This compartment is replete with fibroblasts that can potently enhance HIV infection of resident CD4+ T cells. Stromal fibroblasts from mucosa lined by stratified squamous epithelia similarly enhance HIV infection.
